 The following is an informational post on the disease SMA (spinal muscle atrophy) by Rose Ann Kesting M.A. CCC-SLP. After reading, please visit her blog post “My Wednesday Morning Wake Up Call,” for a personal account of her experience with a very special boy with Type 1 SMA and his amazingly dedicated family. Continue reading Spotlight on Syndromes: An SLPs Perspective on Spinal Muscle Atrophy
The following is an informational post on the disease SMA (spinal muscle atrophy) by Rose Ann Kesting M.A. CCC-SLP. After reading, please visit her blog post “My Wednesday Morning Wake Up Call,” for a personal account of her experience with a very special boy with Type 1 SMA and his amazingly dedicated family. Continue reading Spotlight on Syndromes: An SLPs Perspective on Spinal Muscle Atrophy
Search Results for: Picture books
Birthday Giveaway Day Seventeen: Halloween Language Activity Pack
 It’s DAY 17 of my Birthday Month Giveaways and I am raffling off a giveaway by Kids Games for Speech Therapy which is a Halloween: Language Activity Pack for preschool children. This adorable Halloween themed packet targets the following skills:
It’s DAY 17 of my Birthday Month Giveaways and I am raffling off a giveaway by Kids Games for Speech Therapy which is a Halloween: Language Activity Pack for preschool children. This adorable Halloween themed packet targets the following skills:
- Pronouns (he / she / they / his / hers / theirs / him / her / them)
- Prepositions (on / under / next to / behind / in front)
- Following Multistep Directions
- New Vocabulary Introduction
The pack contains baseboards, picture prompt cards, cutouts, and written cue cards. Detailed SLP and parent instruction sheets are included. The pictures are adorable and very engaging.
You can find this product in Kids Games for Speech Therapy TPT store by clicking HERE or you can enter my one day giveaway for a chance to win.
a Rafflecopter giveaway
Birthday Extravaganza Day Twenty Seven: Elementary My Dear, Analogies
 It’s DAY 27 of my Birthday Month Giveaways and I am raffling off a giveaway by Straight Up Speech, which is Elementary, My Dear Analogies.
It’s DAY 27 of my Birthday Month Giveaways and I am raffling off a giveaway by Straight Up Speech, which is Elementary, My Dear Analogies.
This adorable 12-page critical thinking packet targets early analogies and uses child-friendly graphics to engage students in filling-in-the missing answers.
Packet Contents: Continue reading Birthday Extravaganza Day Twenty Seven: Elementary My Dear, Analogies
In case you missed it: Integrating aspects of multiculturalism into group language therapy sessions
 Last week I did a guest post for The Practically Speeching Blog on the topic of multiculturalism. In case you missed it, below I offer some suggestions on how to integrate multiculturalism into your group therapy sessions.
Last week I did a guest post for The Practically Speeching Blog on the topic of multiculturalism. In case you missed it, below I offer some suggestions on how to integrate multiculturalism into your group therapy sessions.
I don’t know about you but I have a number of multicultural students on my caseload who exhibit language deficits in both their birth language as well as English. Even though I am unable to speak their languages (e.g., Spanish, Hindu) I still like to integrate various aspects of multiculturalism into my sessions in order to support their first language as well as educate them about their culture and other cultures around the world as much as possible. Why? Because among other benefits (e.g., cognitive, linguistic, academic, just to name a few) studies have also found a connection between bilingualism/multiculturalism and higher self-esteem in children (Verkuyten, 2009). For me the latter definitely plays a huge part, since children with language impairments already recognize that they are different from their peers when it comes to their abilities and accomplishments in the classroom, which is why I try to support them in any way that I can in this area. Believe it or not it’s not as complicated as it sounds, and with a little ingenuity you can make it happen as well. Below are some suggestions of what you can do in sessions. Continue reading In case you missed it: Integrating aspects of multiculturalism into group language therapy sessions
Review and Giveaway: Test of Semantic Reasoning (TOSR)
 Today I am reviewing a new receptive vocabulary measure for students 7-17 years of age, entitled the Test of Semantic Reasoning (TOSR) created by Beth Lawrence, MA, CCC-SLP and Deena Seifert, MS, CCC-SLP, available via Academic Therapy Publications.
Today I am reviewing a new receptive vocabulary measure for students 7-17 years of age, entitled the Test of Semantic Reasoning (TOSR) created by Beth Lawrence, MA, CCC-SLP and Deena Seifert, MS, CCC-SLP, available via Academic Therapy Publications.
The TOSR assesses the student’s semantic reasoning skills or the ability to nonverbally identify vocabulary via image analysis and retrieve it from one’s lexicon.
According to the authors, the TOSR assesses “breadth (the number of lexical entries one has) and depth (the extent of semantic representation for each known word) of vocabulary knowledge without taxing expressive language skills”.
The test was normed on 1117 students ranging from 7 through 17 years of age with the norming sample including such diagnoses as learning disabilities, language impairments, ADHD, and autism. This fact is important because the manual did indicate how the above students were identified. According to Peña, Spaulding and Plante (2006), the inclusion of children with disabilities in the normative sample can negatively affect the test’s discriminant accuracy (separate typically developing from disordered children) by lowering the mean score, which may limit the test’s ability to diagnose children with mild disabilities.
TOSR administration takes approximately 20 minutes or so, although it can take a little longer or shorter depending on the child’s level of knowledge. It is relatively straightforward. You start at the age-based point and then calculate a basal and a ceiling. For a basal rule, if the child missed any of the first 3 items, the examiner must go backward until the child retains 3 correct responses in a row. To attain a ceiling, test administration can be discontinued after the student makes 6 out of 8 incorrect responses.
Test administration is as follows. Students are presented with 4 images and told 4 words which accompany the images. The examiner asks the question: “Which word goes with all four pictures? The words are…“
Students then must select the single word from a choice of four that best represents the multiple contexts of the word represented by all the images.
According to the authors, this assessment can provide “information on children and adolescents basic receptive vocabulary knowledge, as well as their higher order thinking and reasoning in the semantic domain.”
My impressions:
During the time I had this test I’ve administered it to 6 students on my caseload with documented history of language disorders and learning disabilities. Interestingly all students with the exception of one had passed it with flying colors. 4 out of 6 received standard scores solidly in the average range of functioning including a recently added to the caseload student with significant word-finding deficits. Another student with moderate intellectual disability scored in the low average range (18th percentile). Finally, my last student scored very poorly (1st%); however, in addition to being a multicultural speaker he also had a significant language disorder. He was actually tested for a purpose of a comparison with the others to see what it takes not to pass the test if you will.
I was surprised to see several children with documented vocabulary knowledge deficits to pass this test. Furthermore, when I informally used the test and asked them to identify select vocabulary words expressively or in sentences, very few of the children could actually accomplish these tasks successfully. As such it is important for clinicians to be aware of the above finding since receptive knowledge given multiple choices of responses does not constitute spontaneous word retrieval.
Consequently, I caution SLPs from using the TOSR as an isolated vocabulary measure to qualify/disqualify children for services, and encourage them to add an informal expressive administration of this measure in words in sentences to get further informal information regarding their students’ expressive knowledge base.
I also caution test administration to Culturally and Linguistically Diverse (CLD) students (who are being tested for the first time vs. retesting of CLD students with confirmed language disorders) due to increased potential for linguistic and cultural bias, which may result in test answers being marked incorrect due lack of relevant receptive vocabulary knowledge (in the absence of actual disorder).
Final Thoughts:
I think that SLPs can use this test as a replacement for the Receptive One-Word Picture Vocabulary Test-4 (ROWPVT-4) effectively, as it does provide them with more information regarding the student’s reasoning and receptive vocabulary abilities. I think this test may be helpful to use with children with word-finding deficits in order to tease out a lack of knowledge vs. a retrieval issue.
You can find this assessment for purchase on the ATP website HERE. Finally, due to the generosity of one of its creators, Deena Seifert, MS, CCC-SLP, you can enter my Rafflecopter giveaway below for a chance to win your own copy!
Disclaimer: I did receive a complimentary copy of this assessment for review from the publisher. Furthermore, the test creators will be mailing a copy of the test to one Rafflecopter winner. However, all the opinions expressed in this post are my own and are not influenced by the publisher or test developers.
References:
Peña ED, Spaulding TJ, and Plante E. ( 2006) The composition of normative groups and diagnostic decision-making: Shooting ourselves in the foot. American Journal of Speech-Language Pathology 15: 247–54
Dear Neurodevelopmental Pediatrician: Please Don’t Do That!
 Recently I got yet another one of the dreaded phone calls which went a little something like this:
Recently I got yet another one of the dreaded phone calls which went a little something like this:
Parent: Hi, I am looking for a speech therapist for my son, who uses PROMPT to treat Childhood Apraxia of Speech (CAS). Are you PROMPT certified?
Me: I am PROMPT trained and I do treat motor speech disorders but perhaps you can first tell me a little bit about your child? What is his age? What type of speech difficulties does he have? Who diagnosed him and recommended the treatment.
Parent: He is turning 3. He was diagnosed by a neurodevelopmental pediatrician a few weeks ago. She recommended speech therapy 4 times a week for 30 minutes sessions, using PROMPT.
Me: And what did the speech therapy evaluation reveal?
Parent: We did not do a speech therapy evaluation yet.
Sadly I get these type of phone calls at least once a month. Frantic parents of toddlers aged 18 months to 3+ years of age call to inquire regarding the availability of PROMPT therapy based exclusively on the diagnosis of the neurodevelopmental pediatrician. In all cases I am told that the neurodevelopmental pediatrician specified speech language diagnosis, method of treatment, and therapy frequency, ALBEIT in a complete absence of a comprehensive speech language evaluation and/or past speech language therapy treatments.
The conversation that follows is often an uncomfortable one. I listen to the parental description of the child’s presenting symptoms and explain to the parents that a comprehensive speech language assessment by a certified speech language pathologist is needed prior to initiation of any therapy services. I also explain to the parents that depending on the child’s age and the assessment findings CAS may or may not be substantiated since there are a number of speech sound disorders which may have symptoms similar to CAS.
Following my ‘spiel’, the parents typically react in a number of ways. Some get offended that I dared to question the judgement of a highly qualified medical professional. Others hurriedly thank me for my time and resoundingly hang up the phone. Yet a number of parents will stay on the line, actually listen to what I have to say and ask me detailed questions. Some of them will even become clients and have their children undergo a speech language evaluation. Still a number of them will find out that their child never even had CAS! Past misdiagnoses ranged from ASD (CAS was mistaken due to the presence of imprecise speech and excessive jargon related utterances) to severe phonological disorder to dysarthria secondary to CP. Thus, prior to performing a detailed speech language evaluation on the child I had no way of knowing whether the child truly presented with CAS symptoms.
Before I continue I’d like to provide a rudimentary definition of CAS. Since its identification years ago it has been argued whether CAS is linguistic or motoric in nature with the latest consensus being that CAS is a disorder which disrupts speech motor control and creates difficulty with volitional, intelligible speech production. Latest research also shows that in addition to having difficulty forming words and sentences at the speech level, children with CAS also experience difficulty in the areas of receptive and expressive language, in other words, “pure” apraxia of speech is rare (Hammer, 2007).

This condition NEEDS to be diagnosed by a speech language pathologist! Not only that, due to the disorder’s complexity it is strongly recommended that if parents suspect CAS they should take their child for an assessment with an SLP specializing in assessment and treatment of motor speech disorders. Here’s why.
- CAS has a number of overlapping symptoms with other speech sound disorders (e.g., severe phonological disorder, dysarthria, etc).
- Symptoms which may initially appear as CAS may change during the course of intervention by the time the child is older (e.g., 3 years of age) which is why diagnosing toddlers under 3 years of age is very problematic and the use of “suspected” or “working” diagnosis is recommended (Davis & Velleman, 2000) in order to avoid misdiagnosis
- Diagnosis of CAS is also problematic due to the fact that there are no valid or reliable standardized assessments sensitive to CAS (McCauley & Strand, 2008). However, a new instrument Dynamic Evaluation of Motor Speech Skill (DEMSS) (Strand et al, 2013) is showing promise with respect to differential diagnosis of severe speech impairments in children
- Thus for children with less severe impairments SLPs need to design tasks to assess the child’s:
- Automatic vs. volitional control
- Simple vs. complex speech
- Consistency of productions on repetitions of same word
- Vowel productions
- Imitation abilities
- Prosody
- Phonetic inventory BEFORE and AFTER intervention
- Types and levels of cueing the child is presently stimulable to
- in order to determine where the breakdown is taking place (Caspari, 2012)
These are just some of the reasons why specialization in CAS is needed and why it is IMPOSSIBLE to make a reliable CAS diagnosis by simply observing the child for a length of time, from a brief physical exam, and from extensive parental interviews (e.g., a typical neurodevelopmental appointment).
In fact, leading CAS experts state that you DON’t need a neurologist in order to confirm the CAS diagnosis (Hammer, 2007).
Furthermore, “NO SINGLE PROGRAM WORKS FOR ALL CHILDREN WITH APRAXIA!!” (Hammer, 2007). Hence SLPs NEED to individualize not only their approach with each child but also switch approaches with the same child when needed it in order to continue making therapy gains. Given the above the PROMPT approach may not even be applicable to some children.
It goes without saying that MANY developmental pediatricians will NOT do this!
But for those who do, I implore you – if you observe that a young child is having difficulty producing speech, please refer the child for a speech language assessment first. Please specify to the parents your concerns (e.g., restricted sound repertoire for the child’s age, difficulty sequencing sounds to make words, etc) BUT NOT the diagnosis, therapy frequency, as well as therapy approaches. Allow the assessing speech language pathologist to make these recommendations in order to ensure that the child receives the best possible targeted intervention for his/her disorder.
For more information please visit the Childhood Apraxia of Speech Association of North America (CASANA) website or visit the ASHA website to find a professional specializing in the diagnosis and treatment of CAS near you.
References:
- Caspari, S (2012) Beyond Picture Cards! Practical Assessment and Treatment Methods for Children with Apraxia of Speech. Session presented for New Jersey Speech Language Hearing Association Convention, Long Branch, NJ
- Davis, B., & Velleman, S. L. (2000). Differential diagnosis and treatment of developmental apraxia of speech in infants and toddlers. Infant-Toddler Intervention: The Transdisciplinary Journal, 10, 177–192.
- Hammer, D (2007) Childhood Apraxia of Speech: Evaluation and Therapy Challenges. Retrieved from http://www.maxshouse.com.au/documents/CAS%20conference%20day%201%20.ppt.
- McCauley RJ, Strand EA. (2008). A Review of Standardized Tests of Nonverbal Oral and Speech Motor Performance in Children. American Journal of Speech-Language Pathology, 17,81-91.
- Strand, E, McCauley, R, Weigand, S, Stoeckel, R & Baas, B (2013) A Motor Speech Assessment for Children with Severe Speech Disorders: Reliability and Validity Evidence. Journal of Speech Language and Hearing Research, vol 56; 505-520.
What Should be Driving Our Treatment?
 Today I want to talk treatment. That thing that we need to plan for as we are doing our assessments. But are we starting our treatments the right way? The answer may surprise you. I often see SLPs phrasing questions regarding treatment the following way: “I have a student diagnosed with ____ (insert disorder here). What is everyone using (program/app/materials) during therapy sessions to address ___ diagnosis?”
Today I want to talk treatment. That thing that we need to plan for as we are doing our assessments. But are we starting our treatments the right way? The answer may surprise you. I often see SLPs phrasing questions regarding treatment the following way: “I have a student diagnosed with ____ (insert disorder here). What is everyone using (program/app/materials) during therapy sessions to address ___ diagnosis?”
Of course, the answer is never that simple. Just because a child has a diagnosis of a social communication disorder, word-finding deficits, or a reading disability does not automatically indicate to the treating clinician, which ‘cookie cutter’ materials and programs are best suited for the child in question. Only a profile of strengths and needs based on a comprehensive language and literacy testing can address this in an adequate and targeted manner.
To illustrate, reading intervention is a much debated and controversial topic nowadays. Everywhere you turn there’s a barrage of advice for clinicians and parents regarding which program/approach to use. Barton, Wilson, OG… the well-intentioned advice just keeps on coming. The problem is that without knowing the child’s specific deficit areas, the application of the above approaches is quite frankly … pointless.
 There could be endless variations of how deficits manifest in poor readers. Is it aspects of phonological awareness, phonics, morphology, etc. What combination of deficits is preventing the child from becoming a good reader?
There could be endless variations of how deficits manifest in poor readers. Is it aspects of phonological awareness, phonics, morphology, etc. What combination of deficits is preventing the child from becoming a good reader?
Let’s a take a look at an example, below. It’s the CTOPP-2 results of a 7-6-year-old female with a documented history of extensive reading difficulties and a significant family history of reading disabilities in the family.
Results of the Comprehensive Test of Phonological Processing-2 (CTOPP-2)
| Subtests | Scaled Scores | Percentile Ranks | Description |
| Elision (EL) | 7 | 16 | Below Average |
| Blending Words (BW) | 13 | 84 | Above Average |
| Phoneme Isolation (PI) | 6 | 9 | Below Average |
| Memory for Digits (MD) | 8 | 25 | Average |
| Nonword Repetition (NR) | 8 | 25 | Average |
| Rapid Digit Naming (RD) | 10 | 50 | Average |
| Rapid Letter Naming (RL) | 11 | 63 | Average |
| Blending Nonwords (BN) | 8 | 25 | Average |
| Segmenting Nonwords (SN) | 8 | 25 | Average |
However, the results of her CTOPP-2 testing clearly indicate that phonological awareness, despite two areas of mild weaknesses, is not really a significant problem for this child. So let’s look at the student’s reading fluency results.
 Reading Fluency: “LG’s reading fluency during this task was judged to be significantly affected by excessive speed, inappropriate pausing, word misreadings, choppy prosody, as well as inefficient word attack skills. While she was able to limitedly utilize the phonetic spelling of unfamiliar words (e.g., __) provided to her in parenthesis next to the word (which she initially misread as ‘__’), she exhibited limited use of metalinguistic strategies (e.g., pre-scanning sentences to aid text comprehension, self-correcting to ensure that the read words made sense in the context of the sentence, etc.), when reading the provided passage. To illustrate, during the reading of the text, LG was observed to frequently (at least 3 times) lose her place and skip entire lines of text without any attempts at self-correction. At times she was observed to read the same word a number of different ways (e.g., read ‘soup’ as ‘soup’ then as ‘soap’, ‘roots’ as ‘roofs’ then as ‘roots’, etc.) without attempting to self-correct. LG’s oral reading rate was also observed to be impaired for her age/grade levels. Her prosody was significantly adversely affected due to lack of adequate pausing for punctuation marks (e.g., periods, commas, etc.). Instead, she paused during text reading only when he could not decode select words in the text. Though, LG was able to read 70 words per minute, which was judged to be grossly commensurate with grade-level, out of these 70 words she skipped 2 entire lines of text, invented an entire line of text, as well as made 4 decoding errors and 6 inappropriate pauses.”
Reading Fluency: “LG’s reading fluency during this task was judged to be significantly affected by excessive speed, inappropriate pausing, word misreadings, choppy prosody, as well as inefficient word attack skills. While she was able to limitedly utilize the phonetic spelling of unfamiliar words (e.g., __) provided to her in parenthesis next to the word (which she initially misread as ‘__’), she exhibited limited use of metalinguistic strategies (e.g., pre-scanning sentences to aid text comprehension, self-correcting to ensure that the read words made sense in the context of the sentence, etc.), when reading the provided passage. To illustrate, during the reading of the text, LG was observed to frequently (at least 3 times) lose her place and skip entire lines of text without any attempts at self-correction. At times she was observed to read the same word a number of different ways (e.g., read ‘soup’ as ‘soup’ then as ‘soap’, ‘roots’ as ‘roofs’ then as ‘roots’, etc.) without attempting to self-correct. LG’s oral reading rate was also observed to be impaired for her age/grade levels. Her prosody was significantly adversely affected due to lack of adequate pausing for punctuation marks (e.g., periods, commas, etc.). Instead, she paused during text reading only when he could not decode select words in the text. Though, LG was able to read 70 words per minute, which was judged to be grossly commensurate with grade-level, out of these 70 words she skipped 2 entire lines of text, invented an entire line of text, as well as made 4 decoding errors and 6 inappropriate pauses.”
So now we know that despite quite decent phonological awareness abilities, this student presents with quite poor sound-letter correspondence skills and will definitely benefit from explicit phonics instruction addressing the above deficit areas. But that is only the beginning! By looking at the analysis of specific misreadings we next need to determine what other literacy areas need to be addressed. For the sake of brevity, I can specify that further analysis of this child reading abilities revealed that reading comprehension, orthographic knowledge, as well as morphological awareness were definitely areas that also required targeted remediation. The assessment also revealed that the child presented with poor spelling and writing abilities, which also needed to be addressed in the context of therapy.
Now, what if I also told you that this child had already been receiving private, Orton-Gillingham reading instruction for a period of 2 years, 1x per week, at the time the above assessment took place? Would you change your mind about the program in question?
Well, the answer is again not so simple! OG is a fine program, but as you can see from the above example it has definite limitations and is not an exclusive fit for this child, or for any child for that matter. Furthermore, a solidly-trained in literacy clinician DOES NOT need to rely on just one program to address literacy deficits. They simply need solid knowledge of typical and atypical language and literacy development/milestones and know how to create a targeted treatment hierarchy in order to deliver effective intervention services. But for that, they need to first, thoughtfully, construct assessment-based treatment goals by carefully taking into the consideration the child’s strengths and needs.
So let’s stop asking which approach/program we should use and start asking about the child’s profile of strengths and needs in order to create accurate language and literacy goals based on solid evidence and scientifically-guided treatment practices.
Helpful Resources Pertaining to Reading:
- Earle, G. A., Sayeski, K. L (2017) Systematic Instruction in Phoneme-Grapheme Correspondence for Students With Reading Disabilities. Intervention in School and Clinic. Vol. 52(5) 262–269
- The Florida Center for Reading Research (FCRR)
- Hasbrouck, J. & Tindal, G. A. (2006). Oral reading fluency norms: A valuable assessment tool for reading teachers. The Reading Teacher. 59(7), 636-644.
- O’Connor, R (2017) Reading Fluency and Students With Reading Disabilities: How Fast Is Fast Enough to Promote Reading Comprehension? Journal of Learning Disabilities
- Tolman, C (2005) Working Smarter, Not Harder: What Teachers of Reading Need to Know and Be Able to Teach IDA Perspectives pp. 15-23.
- Toste et al (2016) Reading Big Words: Instructional Practices to Promote Multisyllabic Word Reading Fluency Intervention in School and Clinic pp. 1–9
- Zipoli, R (2017) Unraveling-Difficult-Sentences: Strategies to Support Reading Comprehension. Intervention in School and Clinic, Vol. 52(4) 218–227. Intervention in School and Clinic, Vol. 52(4) 218–227
The End of See it, Zap it! Ankyloglossia (Tongue-Tie) Controversies in Research and Clinical Practice
 Today it is my pleasure and privilege to interview 3 Australian lactation consultations: Lois Wattis, Renee Kam, and Pamela Douglas, the authors of a March 2017 article in the Breastfeeding Review: “Three experienced lactation consultants reflect upon the oral tie phenomenon” (which can be found HERE).
Today it is my pleasure and privilege to interview 3 Australian lactation consultations: Lois Wattis, Renee Kam, and Pamela Douglas, the authors of a March 2017 article in the Breastfeeding Review: “Three experienced lactation consultants reflect upon the oral tie phenomenon” (which can be found HERE).
Tatyana Elleseff: Colleagues, as you very well know, the subject of ankyloglossia or tongue tie affecting breastfeeding and speech production has risen into significant prominence in the past several years. Numerous journal articles, blog posts, as well as social media forums have been discussing this phenomenon with rather conflicting recommendations. Many health professionals and parents are convinced that “releasing the tie” or performing either a frenotomy or frenectomy will lead to significant improvements in speech and feeding.
 Presently, systematic reviews1-3 demonstrate there is insufficient evidence for the above. However, when many professionals including myself, cite reputable research explaining the lack of support of surgical intervention for tongue tie, there has been a pushback on the part of a number of other health professionals including lactation consultants, nurses, dentists, as well as speech-language pathologists stating that in their clinical experience surgical intervention does resolve issues with tongue tie as related to speech and feeding.
Presently, systematic reviews1-3 demonstrate there is insufficient evidence for the above. However, when many professionals including myself, cite reputable research explaining the lack of support of surgical intervention for tongue tie, there has been a pushback on the part of a number of other health professionals including lactation consultants, nurses, dentists, as well as speech-language pathologists stating that in their clinical experience surgical intervention does resolve issues with tongue tie as related to speech and feeding.
So today, given your 33 combined years of practice as lactation consultants I would love to ask your some questions regarding the tongue tie phenomena.
I would like to begin our discussion with a description of normal breastfeeding and what can interfere with it from an anatomical and physiological standpoint for mothers and babies.
 Now, many of this blog’s readers already know that a tongue tie occurs when the connective tissue under the tongue known as a lingual frenulum restricts tongue movement to some degree and adversely affects its function. But many may not realize that children can present with a normal anatomical variant of “ties” which can be completely asymptomatic. Can you please address that?
Now, many of this blog’s readers already know that a tongue tie occurs when the connective tissue under the tongue known as a lingual frenulum restricts tongue movement to some degree and adversely affects its function. But many may not realize that children can present with a normal anatomical variant of “ties” which can be completely asymptomatic. Can you please address that?
Lois Wattis: “Normal” breastfeeding takes time and skill to achieve. The breastfeeding dyad is multifactorial, influenced by maternal breast and nipple anatomy combined with the infant’s facial and oral structures, all of which are highly variable. Mothers who have successfully breastfed the first baby may encounter problems with subsequent babies due to size (e.g., smaller, larger, etc.), be compromised by birth interventions or drugs during labor, or incur birth injuries – all of which can affect the initiation of breastfeeding and progression to a happy and comfortable feeding relationship. Unfortunately, the overview of each dyad’s story can be lost when tunnel vision of either health provider or parents regarding the baby’s oral anatomy is believed to be the chief influencer of breastfeeding success or failure.
Tatyana Elleseff: Colleagues, what do we know regarding the true prevalence of various ‘tongue ties’? Are there any studies of good quality?
 Pamela Douglas: In a literature review in 2005, Hall and Renfrew acknowledged that the true prevalence of ankyloglossia remained unknown, though they estimated 3-4% of newborns.4
Pamela Douglas: In a literature review in 2005, Hall and Renfrew acknowledged that the true prevalence of ankyloglossia remained unknown, though they estimated 3-4% of newborns.4
After 2005, once the diagnosis of posterior tongue-tie (PTT) had been introduced,5, 6 attempts to quantify incidence of tongue-tie have remained of very poor quality, but estimates currently rest at between 4-10%.7
The problem is that there is a lack of definitional clarity concerning the diagnosis of PTT. Consequently, anterior or classic tongue tie CTT is now often conflated with PTT simply as ‘tongue-tie’ (TT).
Tatyana Elleseff: Thank you for clarifying it. In addition to the anterior and posterior tongue tie labels, many parents and professionals also frequently hear the terms lip tie and buccal ties. Is there’s reputable research behind these terms indicating that these ties can truly impact speech and feeding?
Pamela Douglas: Current definitions of ankyloglossia tend to confuse oral and tongue function (which is affected by multiple variables, and in particular by a fit and hold in breastfeeding) with structure (which is highly anatomically variable for both the tongue length and appearance and lingual and maxillary frenula).
For my own purposes, I define CTT as Type 1 and 2 on the Coryllos-Genna-Watson scale.8 In clinical practice, I also find it useful to rate the anterior membrane by the percentage of the undersurface of the tongue into which the membrane connects, applying the first two categories of the Griffiths Classification System.9
There is a wide spectrum of lingual frenula morphologies and elasticities, and deciding where to draw a line between a normal variant and CTT will depend on the clinical judgment concerning the infant’s capacity for pain-free efficient milk transfer. However, that means we need to have an approach to fit and hold that we are confident does optimize pain-free efficient milk transfer and at the moment, research shows that not only do the old ‘hands on’ approach to fit and hold not work, but that baby-led attachment is also not enough for many women. This is why at the Possums Clinic we’ve been working on developing an approach to fit and hold (gestalt breastfeeding) that builds on baby-led attachment but also integrates the findings of the latest ultrasound studies.
I personally don’t find the diagnoses of posterior tongue tie PTT and upper lip tie ULT helpful, and don’t use them. Lois, Renee and myself find that a wide spectrum of normal anatomic lingual and maxillary frenula variants are currently being misdiagnosed as a PTT and ULT, which has worried us and led Lois to initiate the article with Renee.
Tatyana Elleseff: Segueing from the above question: is there an established criterion based upon which a decision is made by relevant professionals to “release” the tie and if so can you explain how it’s determined?
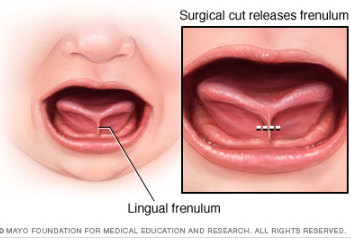 Lois Wattis: When an anterior frenulum is attached at the tongue tip or nearby and is short enough to cause restriction of lift towards the palate, usually associated with extreme discomfort for the breastfeeding mother, I have no reservations about snipping it to release the tongue to enable optimal function for breastfeeding. If a simple frenotomy is going to assist the baby to breastfeed well it is worth doing, and as soon as possible. What I do encounter in my clinical practice are distressed and disempowered mothers whose baby has been labeled as having a posterior tongue tie and/or upper lip tie which is the cause of current and even future problems. Upon examination, the baby has completely normal oral anatomy and breastfeeding upskilling and confidence building of both mother and baby enables the dyad to go forward with strategies which address all elements of their unique story.
Lois Wattis: When an anterior frenulum is attached at the tongue tip or nearby and is short enough to cause restriction of lift towards the palate, usually associated with extreme discomfort for the breastfeeding mother, I have no reservations about snipping it to release the tongue to enable optimal function for breastfeeding. If a simple frenotomy is going to assist the baby to breastfeed well it is worth doing, and as soon as possible. What I do encounter in my clinical practice are distressed and disempowered mothers whose baby has been labeled as having a posterior tongue tie and/or upper lip tie which is the cause of current and even future problems. Upon examination, the baby has completely normal oral anatomy and breastfeeding upskilling and confidence building of both mother and baby enables the dyad to go forward with strategies which address all elements of their unique story.
Although the Hazelbaker Assessment Tool for Lingual Frenulum Function (ATLFF) is a pioneering contribution, bringing us our first systematized approach to examination of the infant’s tongue and oral connective tissues, it is unreliable as a tool for decision-making concerning frenotomy.10-12 In practice many of the item criteria are highly subjective. Although one study found moderate inter-rater reliability on the ATLFF’s structural items, the authors did not find inter-rater reliability on most of the functional items.13 In my clinical experience, there is no reliable correlation between what the tongue is observed to do during oral examinations and what occurs during breastfeeding, other than in the case of classic tongue-tie (excluding congenital craniofacial abnormalities from this discussion.
In my practice as a Lactation Consultant in an acute hospital setting I use a combination of the available assessment tools mainly for documentation purposes, however, the most important tools I use are my eyes and my ears. Observing the mother and baby physical combination and interactions, and suggesting adjustments where indicated to the positioning and attachment technique used (which Pam calls fit and hold) can very often resolve difficulties immediately – even if the baby also has an obvious frenulum under his/her tongue. Listening to the mother’s feedback, and observing the baby’s responses are primary indicators of whether further intervention is needed, or not. Watching how the baby achieves and retains the latch is key, then the examination of baby’s mouth to assess tongue mobility and appearance provide final information about whether baby’s ability to breastfeed comfortably is or is not being hindered by a restrictive lingual frenulum.
Tatyana Elleseff: So frenotomy is an incision (cut) of lingual frenum while frenectomy (complete removal) is an excision of lingual frenum. Both can be performed via various methods of “release”. What effects on breastfeeding have you seen with respect to healing?
Lois Wattis: The significant difference between both procedures involves the degree of invasiveness and level of pain experienced during and after the procedures, and the differing time it takes for the resumption and/or improvement in breastfeeding comfort and efficacy.
It is commonplace for a baby who has had a simple incision to breastfeed immediately after the procedure and exhibit no further signs of discomfort or oral aversion. Conversely, the baby who has had laser division(s) may breastfeed soon after the procedure while topical anesthetics are still working. However, many infants demonstrate discomfort, extreme pain responses and reluctance to feed for days or weeks following a laser treatment. Parents are warned to expect delays resuming feeding and the baby is usually also subjected to wound “stretches” for weeks following the laser treatments. Unfortunately, in my clinical practice I see many parents and babies who are very traumatized by this whole process, and in many cases, breastfeeding can be derailed either temporarily or permanently.
 Tatyana Elleseff: Thank you! This is highly relevant information for both health professionals and parents alike. I truly appreciate your clinical expertise on this topic. While we are on the topic of restrictive lingual frenulums can we discuss several recent articles published on surgical interventions for the above? For example (Ghaheri, Cole, Fausel, Chuop & Mace, 2016), recently published the result of their study which concluded that: “Surgical release of tongue-tie/lip-tie results in significant improvement in breastfeeding outcomes”. Can you elucidate upon the study design and its findings?
Tatyana Elleseff: Thank you! This is highly relevant information for both health professionals and parents alike. I truly appreciate your clinical expertise on this topic. While we are on the topic of restrictive lingual frenulums can we discuss several recent articles published on surgical interventions for the above? For example (Ghaheri, Cole, Fausel, Chuop & Mace, 2016), recently published the result of their study which concluded that: “Surgical release of tongue-tie/lip-tie results in significant improvement in breastfeeding outcomes”. Can you elucidate upon the study design and its findings?
Pamela Douglas: Pre-post surveys, such as Ghaheri et al’s 2016 study, are notoriously methodologically weak and prone to interpretive bias.14
Renee Kam: Research about the efficacy of releasing ULTs to improve breastfeeding outcomes is seriously lacking. There is no reliable assessment tool for upper lip-tie and a lack of evidence to support the efficacy of a frenotomy of labial frenula in breastfed babies. The few studies which have included ULT release have either included very small numbers of babies having upper lip-tie releases or have included babies having a release upper lip ties and tongue ties at the same time, making it impossible to know if any improvements were due to the tongue-tie release, upper lip-tie release or both. Here, to answer your previous question, to date, no research has looked into the treatment of buccal ties for breastfeeding outcomes.
There are various classification scales for labial frenulums such as the Kotlow scale. The title of this scale is misleading as it contains the word ‘tie’. Hence it can give some people the incorrect assumption that a class III or IV labial frenulum is somehow a problem. What this scale actually shows is the normal range of insertion sites for a labial frenulum. And, in normal cases, the vast majority of babies’ labial frenulums insert low down on the upper gum (class III) or even wrap around it (class IV). It’s important to note that, for effective breastfeeding, the upper lip does not have to flange out in order to create a seal. It just has to rest in a neutral position — not flanged out, not tucked in.
Lois Wattis: I entirely agree with Renee’s view about the neutrality of the upper lip, including the labial frenulum, in relation to latch for breastfeeding. Even babies with asymmetrical facial features, cleft lips and other permanent and temporary anomalies only need to achieve a seal with the upper lip to breastfeed successfully.
 Tatyana Elleseff: Thank you for that. In addition to studies on tongue tie revisions and breastfeeding outcomes, there has been an increase in studies, specifically Kotlow (2016) and Siegel (2016), which claimed that surgical intervention improves outcomes for acid reflux and aerophagia in babies”. Can you discuss these studies design and findings?
Tatyana Elleseff: Thank you for that. In addition to studies on tongue tie revisions and breastfeeding outcomes, there has been an increase in studies, specifically Kotlow (2016) and Siegel (2016), which claimed that surgical intervention improves outcomes for acid reflux and aerophagia in babies”. Can you discuss these studies design and findings?
Renee Kam: The AIR hypothesis has led to reflux being used as another reason to diagnose the oral anatomic abnormalities in infants in the presence of breastfeeding problems. More research with objective indicators and less vested interest is needed in this area. A thorough understanding of normal infant behavior and feeding problems which aren’t tie related are also imperative before any conclusions about AIR can be reached.
Tatyana Elleseff: One final question, colleagues are you aware of any studies which describe long-term outcomes of surgical interventions for tongue ties?
Pamela Douglas: The systematic reviews note that there is a lack of evidence demonstrating long-term outcomes of surgical interventions.
Tatyana Elleseff: Thank you for such informative discussion, colleagues.
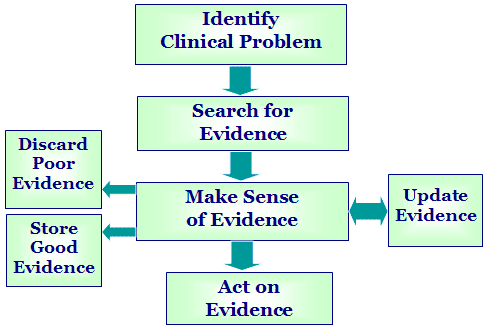 There you have it, readers. Both research and clinical practice align to indicate that:
There you have it, readers. Both research and clinical practice align to indicate that:
- There’s significant normal variation when it comes to most anatomical structures including the frenulum
- Just because a child presents with restricted frenulum does not automatically imply adverse feeding as well as speech outcomes and immediately necessitates a tongue tie release
- When breastfeeding difficulties arise, in the presence of restricted frenulum, it is very important to involve an experienced lactation specialist who will perform a differential diagnosis in order to determine the source of the baby’s true breastfeeding difficulties
Now, I’d like to take a moment and address the myth of tongue ties affecting speech production, which continues to persist among speech-language pathologists despite overwhelming evidence to the contrary.
For that purpose, I will use excerpts from an excellent ASHA Leader December 2005 article written by an esteemed Dr. Kummer who is certainly well qualified to discuss this issue. According to Dr. Kummer, “there is no empirical evidence in the literature that ankyloglossia typically causes speech defects. On the contrary, several authors, even from decades ago, have disputed the belief that there is a strong causal relationship (Wallace, 1963; Block, 1968; Catlin & De Haan, 1971; Wright, 1995; Agarwal & Raina, 2003).”
 Since many children with restricted frenulum do not have any speech production difficulties, Dr Kummer explains why that is the case by discussing the effect of tongue tip positioning for speech production.
Since many children with restricted frenulum do not have any speech production difficulties, Dr Kummer explains why that is the case by discussing the effect of tongue tip positioning for speech production.
“Lingual-alveolar sounds (t, d, n) are produced with the top of the tongue tip and therefore, they can be produced with very little tongue elevation or mobility.
The /s/ and /z/ sounds require the tongue tip to be elevated only slightly but can be produced with little distortion if the tip is down.
The most the tongue tip needs to elevate is to the alveolar ridge for the production of an /l/. However, this sound can actually be produced with the tongue tip down and the dorsum of the tongue up against the alveolar ridge. Even an /r/ sound can be produced with the tongue tip down as long as the back of the tongue is elevated on both sides.
The most the tongue needs to protrude is to the back of the maxillary incisors for the production of /th/. All of these sounds can usually be produced, even with significant tongue tip restriction. This can be tested by producing these sounds with the tongue tip pressed down or against the mandibular gingiva. This results in little, if any, distortion.” (Kummer, 2005, ASHA Leader)
In 2009, Dr. Sharynne McLeod, did research on electropalatography of speech sounds with adults. Her findings (below) which are coronal images of tongue positioning including bracing, lateral contact and groove formation for consonants support the above information provided by Dr. Kummer.
Once again research and clinical practice align to indicate that there’s insufficient evidence to indicate the effect of restricted frenulum on the production of speech sounds.
Finally, I would like to conclude this post with a list of links from recent systematic reviews summarizing the latest research on this topic.
Ankyloglossia/Tongue Tie Systematic Review Summaries to Date (2017):
- A small body of evidence suggests that frenotomy may be associated with mother reported improvements in breastfeeding, and potentially in nipple pain, but with small, short-term studies with inconsistent methodology, the strength of the evidence is low to insufficient.
- In an infant with tongue-tie and feeding difficulties, surgical release of the tongue-tie does not consistently improve infant feeding but is likely to improve maternal nipple pain. Further research is needed to clarify and confirm this effect.
- Data are currently insufficient for assessing the effects of frenotomy on nonbreastfeeding outcomes that may be associated with ankyloglossia
- Given the lack of good-quality studies and limitations in the measurement of outcomes, we considered the strength of the evidence for the effect of surgical interventions to improve speech and articulation to be insufficient.
- Large temporal increases and substantial spatial variations in ankyloglossia and frenotomy rates were observed that may indicate a diagnostic suspicion bias and increasing use of a potentially unnecessary surgical procedure among infants.
References
- Power R, Murphy J. Tongue-tie and frenotomy in infants with breastfeeding difficulties: achieving a balance. Archives of Disease in Childhood 2015;100:489-494.
- Francis DO, Krishnaswami S, McPheeters M. Treatment of ankyloglossia and breastfeeding outcomes: a systematic review. Pediatrics. 2015;135(6):e1467-e1474.
- O’Shea JE, Foster JP, O’Donnell CPF, Breathnach D, Jacobs SE, Todd DA, et al. Frenotomy for tongue-tie in newborn infants (Review). Cochrane Database of Systematic Reviews. 2017 (3):Art. No.:CD011065.
- Hall D, Renfrew M. Tongue tie. Archives of Disease in Childhood. 2005;90:1211-1215.
- Coryllos E, Watson Genna C, Salloum A. Congenital tongue-tie and its impact on breastfeeding. Breastfeeding: Best for Mother and Baby, American Academy of Pediatrics. 2004 Summer:1-6.
- Coryllos EV, Watson Genna C, LeVan Fram J. Minimally Invasive Treatment for Posterior Tongue-Tie (The Hidden Tongue-Tie). In: Watson Genna C, editor. Supporting Sucking Skills. Burlington, MA: Jones and Bartlett Learning; 2013. p. 243-251.
- National Health and Medical Research Council. Infant feeding guidelines: information for health workers. In: Government A, editor. 2012. p. https://www.nhmrc.gov.au/guidelines-publications/n56.
- Watson Genna C, editor. Supporting sucking skills in breastfeeding infants. Burlington, MA: Jones and Bartlett Learning; 2016.
- Griffiths DM. Do tongue ties affect breastfeeding? . Journal of Human Lactation. 2004;20:411.
- Ricke L, Baker N, Madlon-Kay D. Newborn tongue-tie: prevalence and effect on breastfeeding. Journal of American Board of Family Practice. 2005;8:1-8.
- Madlon-Kay D, Ricke L, Baker N, DeFor TA. Case series of 148 tongue-tied newborn babies evaluated with the assessment tool for lingual function. Midwifery. 2008;24:353-357.
- Ballard JL, Auer CE, Khoury JC. Ankyloglossia: assessment, incidence, and effect of frenuloplasty on the breastfeeding dyad. Pediatrics. 2002;110:e63.
- Amir L, James JP, Donath SM. Reliability of the Hazelbaker Assessment Tool for Lingual Frenulum Function. International Breastfeeding Journal. 2006;1:3.
- Douglas PS. Conclusions of Ghaheri’s study that laser surgery for posterior tongue and lip ties improve breastfeeding are not substantiated. Breastfeeding Medicine. 2017;12(3):DOI: 10.1089/bfm.2017.0008.
Author Bios (in alphabetical order):
 Dr. Pamela Douglas is the founder of a charitable organization, the Possums Clinic, a general practitioner since 1987, an IBCLC (1994-2004; 2012-Present) and researcher. She is an Associate Professor (Adjunct) with the Centre for Health Practice Innovation, Griffith University, and a Senior Lecturer with the Discipline of General Practice, The University of Queensland. Pam enjoys working clinically with families across the spectrum of challenges in early life, many complex (including breastfeeding difficulty) unsettled infant behaviors, reflux, allergies, tongue-tie/oral connective tissue problems, and gut problems. She is author of The discontented little baby book: all you need to know about feeds, sleep and crying (UQP) www.possumsonline.com; www.pameladouglas.com.au
Dr. Pamela Douglas is the founder of a charitable organization, the Possums Clinic, a general practitioner since 1987, an IBCLC (1994-2004; 2012-Present) and researcher. She is an Associate Professor (Adjunct) with the Centre for Health Practice Innovation, Griffith University, and a Senior Lecturer with the Discipline of General Practice, The University of Queensland. Pam enjoys working clinically with families across the spectrum of challenges in early life, many complex (including breastfeeding difficulty) unsettled infant behaviors, reflux, allergies, tongue-tie/oral connective tissue problems, and gut problems. She is author of The discontented little baby book: all you need to know about feeds, sleep and crying (UQP) www.possumsonline.com; www.pameladouglas.com.au
 Renee Kam qualified with a Bachelor of Physiotherapy from the University of Melbourne in 2000. She then worked as a physiotherapist for 6 years, predominantly in the areas of women’s health, pediatric and musculoskeletal physiotherapy. She became an Australian Breastfeeding Association Breastfeeding (ABA) counselor in 2010 and obtained the credential of International Board Certified Lactation Consultant (IBCLC) in 2012. In 2013, Renee’s book, The Newborn Baby Manual, was published which covers the topics that Renee is passionate about; breastfeeding, baby sleep and baby behavior. These days, Renee spends most of her time being a mother to her two young daughters, writing breastfeeding content for BellyBelly.com.au, fulfilling her role as national breastfeeding information manager with ABA and working as an IBCLC in private practice and at a private hospital in Melbourne, Australia.
Renee Kam qualified with a Bachelor of Physiotherapy from the University of Melbourne in 2000. She then worked as a physiotherapist for 6 years, predominantly in the areas of women’s health, pediatric and musculoskeletal physiotherapy. She became an Australian Breastfeeding Association Breastfeeding (ABA) counselor in 2010 and obtained the credential of International Board Certified Lactation Consultant (IBCLC) in 2012. In 2013, Renee’s book, The Newborn Baby Manual, was published which covers the topics that Renee is passionate about; breastfeeding, baby sleep and baby behavior. These days, Renee spends most of her time being a mother to her two young daughters, writing breastfeeding content for BellyBelly.com.au, fulfilling her role as national breastfeeding information manager with ABA and working as an IBCLC in private practice and at a private hospital in Melbourne, Australia.
 Lois Wattis is a Registered Nurse/Midwife, International Board Certified Lactation Consultant and Fellow of the Australian College of Midwives. Working in both hospital and community settings, Lois has enhanced her midwifery skills and expertise by providing women-centred care to thousands of mothers and babies, including more than 50 women who chose to give birth at home. Lois’ qualifications include Bachelor of Nursing Degree (Edith Cowan University, Perth WA), Post Graduate Diploma in Clinical Nursing, Midwifery (Curtin University, Perth WA), accreditation as Independent Practising Midwife by the Australian College of Midwives in 2002 and International Board Certified Lactation Consultant in 2004. Lois was inducted as a Fellow of the Australian College of Midwives (FACM) in 2005 in recognition of her services to women and midwifery in Australia. Lois has authored numerous articles which have been published internationally in parenting and midwifery journals, and shares her broad experience via her creations “New Baby 101” book, smartphone App, on-line videos and Facebook page. www.newbaby101.com.au Lois has worked for the past 10 years in Qld, Australia in a dedicated Lactation Consultant role as well as in private practice www.birthjourney.com
Lois Wattis is a Registered Nurse/Midwife, International Board Certified Lactation Consultant and Fellow of the Australian College of Midwives. Working in both hospital and community settings, Lois has enhanced her midwifery skills and expertise by providing women-centred care to thousands of mothers and babies, including more than 50 women who chose to give birth at home. Lois’ qualifications include Bachelor of Nursing Degree (Edith Cowan University, Perth WA), Post Graduate Diploma in Clinical Nursing, Midwifery (Curtin University, Perth WA), accreditation as Independent Practising Midwife by the Australian College of Midwives in 2002 and International Board Certified Lactation Consultant in 2004. Lois was inducted as a Fellow of the Australian College of Midwives (FACM) in 2005 in recognition of her services to women and midwifery in Australia. Lois has authored numerous articles which have been published internationally in parenting and midwifery journals, and shares her broad experience via her creations “New Baby 101” book, smartphone App, on-line videos and Facebook page. www.newbaby101.com.au Lois has worked for the past 10 years in Qld, Australia in a dedicated Lactation Consultant role as well as in private practice www.birthjourney.com
Articulation Assessment ToolKt
 In February 2013 I did a review of the Sunny Articulation Test by Smarty Apps. At that time I really liked the test but felt that a few enhancements could really make it standout from other available articulation tests and test apps on the market. Recently, the developer, Barbara Fernandes, contacted me again and asked me to take a second look at the new and improved Sunny Articulation and Phonology Kit (SAPT-K), which is what I am doing today. Continue reading Articulation Assessment ToolKt
In February 2013 I did a review of the Sunny Articulation Test by Smarty Apps. At that time I really liked the test but felt that a few enhancements could really make it standout from other available articulation tests and test apps on the market. Recently, the developer, Barbara Fernandes, contacted me again and asked me to take a second look at the new and improved Sunny Articulation and Phonology Kit (SAPT-K), which is what I am doing today. Continue reading Articulation Assessment ToolKt
App Review and Giveaway: Between the Lines Level 2
 I enjoyed reviewing Between the Lines Advanced so much that today I am bringing you an intermediate version of this awesome social-pragmatic language app called: Between the Lines Level 2, which also focuses on targeting: Interpretation of vocal tone, Recognition of facial expressions, Interpretation of body language as well as Recognition of idiomatic expressions and slang, just on a less advanced level and in a less challenging format. The app uses photos and mini videos of people in a variety of real-life dynamic social situations to teach social skills. Continue reading App Review and Giveaway: Between the Lines Level 2
I enjoyed reviewing Between the Lines Advanced so much that today I am bringing you an intermediate version of this awesome social-pragmatic language app called: Between the Lines Level 2, which also focuses on targeting: Interpretation of vocal tone, Recognition of facial expressions, Interpretation of body language as well as Recognition of idiomatic expressions and slang, just on a less advanced level and in a less challenging format. The app uses photos and mini videos of people in a variety of real-life dynamic social situations to teach social skills. Continue reading App Review and Giveaway: Between the Lines Level 2
