 Today’s guest post on genetic syndromes comes from Amy Locy, who is contributing an informative piece on the Treacher Collins Syndrome (TCS). TSC occurs in 1 out of every 50,000 live births with 40% of children born with TCS having a family member with the syndrome. TCS is distributed equally across genders and races. It can often occur in conjunction with the Pierre Robin Sequence.
Today’s guest post on genetic syndromes comes from Amy Locy, who is contributing an informative piece on the Treacher Collins Syndrome (TCS). TSC occurs in 1 out of every 50,000 live births with 40% of children born with TCS having a family member with the syndrome. TCS is distributed equally across genders and races. It can often occur in conjunction with the Pierre Robin Sequence.
Developmental Anomalies
There are many developmental anomalies associated with TCS that are restricted to the head and neck and vary from person to person.
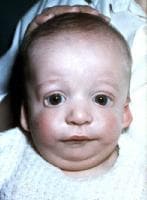
Facial abnormalities of TCS include: hypoplasia of the facial bones, particularly the mandible and zygomatic complex, a narrow face with increased anterior facial height, micrognathia, and macrostomia.
Oral traits that are specific to TCS may include: decreased oral cavity dimension, pharyngeal hypoplasia, and a high arched palate, malocclusion (typically an anterior open bite), severe dysplasia of the temporomandibular joint and tooth abnormalities.
About 35% of people with TCS have cleft palate, and an additional 30-40% of people have velopharyngeal insufficiency (Horbelt, 2012). In rare cases people may present with cleft lip and palate. There are also eye abnormalities including palpebral fissures, hypertelorism, and coloboma.
Many people with TCS also have both internal and external ear abnormalities which may include microtia and/or atresia, and in many cases results in a bilateral conductive hearing loss. Babies born with TCS may also have Pierre Robin Sequence (PRS) which is characterized by glossoptosis, a wide U-shaped cleft palate, and micrognathia (Kummer, 2008).
These physical malformations also carry with them many related conditions such as airway obstruction, sleep apnea, feeding difficulties, and hearing loss. People with TCS must endure a multitude of reconstructive surgeries that are rarely fully corrective. Effects of TCS are not limited to physical complications; craniofacial deformities can have a huge impact on psychological well-being and social interactions.
There are several health concerns in people with TCS that result from the structural abnormalities of the head and neck. Obstructive Sleep Apnea (OSA) is very common in people with TCS due to micrognathia and the narrowing of the airway that may be caused by hypoplasia of the mandible and zygomatic complex, cleft palate, and choanal atresia.
OSA is caused by obstruction to the upper airways during sleep despite inspiratory effort which leads to oxygen desaturation and sleep disruption. OSA is not correlated to severity of TCS but poses a huge health risk for individuals. It affect cognitive function and in severe cases result in death so detection and management of this condition is critical. Medical management includes use of continuous positive airway pressure (CPAP) in children and corrective surgery of the mandible in adults (Akre, Overland, Asten, Skogedal, & Heimdal, 2011).
Behavioral Manifestations
Once the infant reaches childhood they may develop a fear of hospitalization that can be manifested in their behavior. Talking with a mental health professional preoperatively can help alleviate some of these anxieties because the professional, such as a child life therapist, is trained in helping children make sense of what is going on and cope with this type of stress.
Parents may also fear their child undergoing surgical interventions which is another reason it is important that a mental health professional is part of the interdisciplinary team. As the child becomes older it is important that they are given a voice in the decision making process about their treatment, and it is important that parents recognize that their child’s concerns and priorities may be different than their own.
Although children with craniofacial deformities such as TCS are at an elevated risk for mental health problems with reconstructive surgery and the care of a mental health professional as these children reach adulthood and the end of their surgical care many of them learn successful coping strategies and have positive mental health outcomes (Pruzinsky, 1990).
Cognitive abnormalities
There are no cognitive effects of TCS in terms of cognitive disability; however there are many psychological consequences of having a craniofacial syndrome.
Speech and Language Issues and Applicable Interventions
Feeding may be a concern in babies born with TCS due to their structural abnormalities. They may also have inefficient oral-motor mechanics for sucking and may require specialized feeding adaptations (Kummer, 2008). If a child has a cleft palate breast feeding is nearly impossible so the infant must be bottle fed with a special bottle or special techniques used by the person feeding the child.
Since Pierre Robin Sequence (PRS) is common in children with TCS they may experience feeding difficulties that are not related to a cleft, but instead related significant retrognathia or micrognatia. Due to this combined with the retracted tongue position in infants with PRS the infant may not be able to adequately compress the nipple.
In some cases, airway complications and cleft palate compound with the feeding difficulties due to the retrognatia and micrognatia and some infants require a feeding tube, or feeding modifications must be made to orally feed the infant. These feeding modifications may include use of special bottles each with their own specific directions for the caregiver providing the feeding (e.g., Haberman feeder, Meade Johnson bottle), different positioning techniques (e.g., prone, sidelying, or semireclined), or supplemental feedings via a nasopharyngeal tube (NP tube).
Bilateral conductive hearing loss is common in TCS and needs to be managed in order to encourage the development of children with TCS. Cosmetic surgery is typically preformed on the ears, but corrective surgery for hearing is not always an option because many people with TCS have internal ear abnormalities as well. Internal and external ear reconstruction, weather is be cosmetic or functional, cannot safely be performed until school-age (Marsella, Scorpecci, Pacifico, & Tieri, 2011).
Speech disorders are common in children with TCS due to hearing loss and micrognathia (Kummer, 2008). Another possible cause for speech and language delays in this population is the extensive time TCS patients spend hospitalized during infancy and early childhood.
Hospitals are not a language rich environment and do not allow for interaction with peers. Early intervention for children with hearing loss is necessary in order to assure appropriate language development. Audiological management of the hearing loss is necessary and one option is the use of bone-anchored hearing aids (Baha).
Babies who are born with TCS may have severe complications with breathing due to the narrowing of the upper airway because of the structural abnormalities of the oral cavity and the presence of a normally sized and sometimes posteriorly positioned tongue. Immediate medical management is needed to ensure the safety of these infants and in severe cases a tracheostomy may be performed.
However, a tracheostomy is a last resort type of procedure due to the profound negative effects it has on speech and swallowing. In children where a tracheostomy is preformed it usually stays in place until after the palate is fixed around 10-12 months of age which inhibits vocalizations and hinders the development of speech and language (Kummer, 2008).
If a tracheostomy is preformed it is very important that the child is fit with a speech valve as soon as possible, even if the child is preverbal since crying (with vocalization) and babbling are not possible without this device. Another way that surgeons may choose to manage the airway obstruction is by mandibular distraction which pulls the mandible forward and increases the airway space up to 14 mm (Hylton, Leon-Salazar, Anderson, & De Felippe, 2012).
Surgical Interventions
Surgical interventions for individuals born with TCS are extensive and begin in infancy and continue through adulthood. The specific surgeries that are needed by each affected individual will vary due to the varying presentation of TCS. According to Hylton, Leon-Salazar, Anderson, and De Felippe (2012) the following is the typically surgical progression that a patient with TCS must undergo.
The first surgeries that many people with TCS undergo are related to their airway and cleft lip and palate if present. Airway management which may include tracheostomy or mandibular distraction occurs between 0-12 months of age. Repair of a cleft lip is typically done between 3-6 weeks of age, and repair of a cleft palate is typically done between 10-12 months of age. If needed VPI surgery, hearing and vision surgeries, choanal atresia surgery, auricular reconstruction and dental treatment under general anesthesia occur between ages 1 and 8 years. Dental extractions take place between 6 and 16 years of age.
Condylar recontouring occurs at age 6-10 years if needed. Secondary alveolar bone grafting occurs between age 9 and 13. Auricular implants typically occur after 10 years of age. Surgically assisted rapid maxillary expansion occurs after 15 years of age and orthognathic surgery and dental implants are typically done once growth has ceased and the patient has grown to their adult size. Soft-tissue esthetic procedures can begin once the patient reaches fourteen years of age, however many patients become burned out on surgery since they experience so many in childhood and opt out of soft-tissue surgeries.
Multidisciplinary Approach:
Due to the extensive involvement of TCS it is ideally treated by an interdisciplinary team of professionals including: an audiologist, speech language pathologist, otorhinolarygngologist, dentist, orthodontist, oral and maxillofacial surgeon, plastic surgeon, ophthalmologist, and psychologist. These professionals work together to ensure comprehensive care for the individual with TCS.
Treacher Collins Syndrome is a genetic craniofacial disorder that presents differently across the affected population. With comprehensive long-term care by a multidisciplinary team people born with TCS typically are able to lead normal lives.
References
Akre, H., Overland, B., Asten, P., Skogedal, N., Heimdal, K. (2011). Obstructive sleep apnea in Treacher Collins syndrome. Eur Arch Otorhinolaryngol. 269, 331-337.
Horbelt, C. (2008). A review of physical, behavioral, and oral characteristics associated with Treacher Collins syndrome, Goldenhar syndrome, and Angelman syndrome. General Dentistry. 416-418.
Hylton, J., Leon-Salazar, V., Anderson, G., De Felippe, N. (2012). Multidisciplinary treatment approach in Treacher Collins syndrome. Journal of Dentistry for Children. 79:1, 15-21.
Marsella, P., Scorpecci, A., Pacifico, C., Tieri, L. (2011). Bone-anchored hearing aid (Baha) in patients with Treacher Collins syndrome: Tips and pitfalls. International Journal of Pediatric Otorhinolaryngology. 75, 1308-1312.
Purzinsky, T. (1990). Collaboration of plastic surgeon and medical psychotherapist: Reconstructive surgery for congenital craniofacial deformities. Medical Pyschotherapy. 3, 103-116.
Trainor, P., Dixon, J., Dixon, M. (2009). Treacher Collins syndrome: etiology, pathogenesis and prevention. European Journal of Human Genetics. 17, 257-283.
Wu, R., Lawson, C., Jabs, E., Sanderson, S. (2012) Attitudes towards prenatal genetic testing for Treacher Collins syndrome among affected individuals and families. American Journal of Medical Genetics Part A. 158A, 1556-1567.
 Amy Locy is a recent graduate from the University of WI-Stevens Point Speech and Language Pathology program. She is currently in her Clinical Fellowship Year working towards her ASHA certification as a school-based speech and language pathologist. She works with students aged 3-21 and loves the diversity of students and needs that she gets to work with every day. During the summer of 2012 she had the opportunity to study abroad in Curitiba, Brazil at a craniofacial anomalies clinic, CAIF. According to Amy: I learned more about craniofacial disorders and the amazing results a team of professionals can have when they work collaboratively with one another in the two weeks she studied in Brazil than I did in several years of reading textbooks on the subject”.
Amy Locy is a recent graduate from the University of WI-Stevens Point Speech and Language Pathology program. She is currently in her Clinical Fellowship Year working towards her ASHA certification as a school-based speech and language pathologist. She works with students aged 3-21 and loves the diversity of students and needs that she gets to work with every day. During the summer of 2012 she had the opportunity to study abroad in Curitiba, Brazil at a craniofacial anomalies clinic, CAIF. According to Amy: I learned more about craniofacial disorders and the amazing results a team of professionals can have when they work collaboratively with one another in the two weeks she studied in Brazil than I did in several years of reading textbooks on the subject”.
Thank you for this interesting and informative post. I once worked with an adult with TCS. He had autism also we think and a diagnosis of moderate /severe intellectual disability . He had a fascinating personal space construct, would only allow me to come a certain set distance near him . He only ever learned one sign with Lámh ( modified sign language) , thank you. We were working on more signs when he passed away prematurely . This post straight away reminded me of
Him